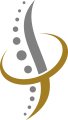
Your spine is a column of bones, called vertebrae, that are stacked on top of one another. In between each of the vertebrae is a spongy disc that serves as a cushion and shock absorber. Your discs prevent the vertebrae from rubbing against each other and they allow the spine to move freely while remaining in proper alignment. These intervertebral discs consist of a gel-like center that is surrounded by a tough outer ring of fibers. When the soft interior of the disc pushes or migrates out of the exterior shell and into the spinal canal, it’s referred to as disc herniation, sometimes called a “slipped disc,” “bulging disc,” or “ruptured disc.”
Symptoms of a Herniated Disc
Herniated discs usually occur in the lumbar spine (lower back) and are a leading cause of lower back pain and sciatica. Disc herniation can take place in the cervical spine (neck), too. The herniated disc may put pressure on the spinal cord or nearby nerves, leading to pain and neurological symptoms.

Common symptoms of disc herniation include:
Mild to severe pain in the lower back or neck
At the onset of the condition, neck or lower back pain sometimes lasts for a few days and then seems to get better. However, as the problem worsens, your pain will become more persistent, lasting for longer periods. The pain is usually exacerbated by movement.
Tingling or numbness
Tingling, a feeling of “pins and needles,” numbness or a burning sensation in the leg or foot is an indication of a herniated lumbar disc. A herniated disc in the neck can cause similar sensations in the shoulder, arm or hand.
Pain in Your Arms or Legs
Depending on the location of the herniation, you may experience radiating or shooting pain that travels down the buttock and through the leg (sciatica) or down the shoulder and arm. The pain gets more intense with activity.
Weakness in the arm or leg
Weakness in your arm or leg is another sign of a herniated disc. This can make it difficult to walk and to lift, push or pull objects. In severe cases, muscle atrophy occurs.
Loss of bladder or bowel control
Rarely, you can lose control of the bladder or bowel. This is a sign that disc herniation is in its advanced stages and may require surgery.
Risk Factors and Causes of Disc Herniation
Aging
Wear and tear on the vertebral discs happens as part of the normal aging process. The discs may dry out, become less pliable and lose strength, which causes the distance between each vertebrae to narrow and makes the discs more susceptible to tearing and rupture.
Improper and/or Repetitive Lifting
When lifting objects, particularly heavy objects, it’s crucial to let the supportive muscles of the legs do the bulk of the work. Improper lifting using your back muscles boosts your risk of disc herniation.
Gender
Herniated discs are more common in men than women. Men between the ages of 30 and 50 are especially prone to disc herniation.
Occupation
People with physically demanding jobs have a higher risk of developing a herniated disc.
Sedentary Lifestyle
Prolonged sitting and a sedentary lifestyle can impact your spine health and lead to disc herniation.
Weight
Being overweight or obese puts more stress on the spine and can hasten the degeneration of the discs.
Genetics
The chances that you’ll develop one or more herniated discs at some point in your life increases if you have a family history of degenerative disc diseases.
Spinal Injury
Excessive force to the spine, such as from a collision or fall, can result in disc herniation.

How is a Herniated Disc Diagnosed?
Discussion With Dr. Choi
During your consultation at Spine Medicine & Surgery of Long Island, Dr. Choi will thoroughly review your symptoms with you and discuss your medical and spine health history.
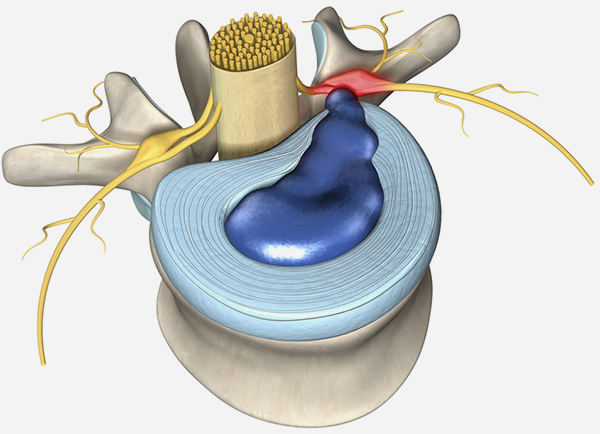
Exam
Our Long Island spine surgeon will perform a physical examination of your back and test your range of motion.
Imaging and Diagnostic Tests
Dr. Choi will likely order an x-ray, MRI and/or CT scan. He might also recommend specialized nerve tests if he needs to pinpoint the location of possibly affected nerves or if he thinks another condition may be involved with your disc herniation.
Herniated Disc Treatment
Once Dr. Choi confirms that a herniated disc is at the root of your symptoms, he’ll create a personalized treatment plan. Many patients heal on their own in several months with a combination of physical therapy, rest and over-the-counter non-steroidal anti-inflammatory medications (NSAIDs).
If your herniated disc does not improve, the next step is usually steroid injections and/or prescription medication to reduce pain and encourage healing. After exhausting these conservative measures, if your symptoms haven’t improved or they get worse, Dr. Choi may recommend surgery for the herniated disc. He’ll explain the procedure in detail, including the risks, benefits and what to expect.
Herniated Disc Surgery
As a top Long Island spine surgeon specializing in minimally invasive techniques, Dr. Choi offers a range of state-of-the-art procedures to treat disc herniation. If the herniated disc is compressing the spinal nerve, surgery to remove the damaged portion of the disc can eliminate the source of your pain and help your body heal.
Spinal fusion is another option for some patients. During this surgery, Dr. Choi removes nerve compression. He then fuses two or more vertebrae together into one continuous bone using bone grafts and metal rods and screws. This alleviates pain, stabilizes the spine and helps you regain most of your range of motion.
For severe disc degeneration, total disc replacement could be the ideal solution. Dr. Choi removes the herniated disc and inserts an artificial disc in its place. This approach offers freedom from pain without compromising function or mobility.
Less Pain, More Living
Find out how we can help you achieve freedom from pain. To get started, schedule a consultation with our Long Island spine surgeon today!